Spondylosis Deformans – Canine
Patient
Labrador, MN, 13 year-old (Fig. 1)
History
The patient was presented for an annual geriatric wellness exam with no owner complaints.
Physical Examination
No significant findings for a geriatric patient. No pain was noted during the examination.
Physiological Screen with Digital Thermal Imaging
The patient was acclimated to room temperature, was not handled during acclimation, and remained calm during image capture. A standard set of 10 digital thermal images were captured with a Digatherm IR camera.
Evaluation of the Thermal Images
All anatomical areas of the patient were thermally symmetrical except for thermal asymmetry within the thoracic paravertebral musculature and scapular regions (Fig. 2).
The abnormalities included:
- A hyperthermic area over the right thoracic paravertebral musculature extending from T6-T10 with a significant focal increase in the thermal gradient from T6-T8.
- Two asymmetrical areas over the left paravertebral musculature extending from T4-T6. A small focal area of hypothermia left lateral to T4 accompanied by a focal area of hyperthermia left lateral to T6.
- Asymmetrical disseminating hyperthermia posterior to a focal hyperthermia over the dorsocaudal right scapula.
- Areas of asymmetrical hypothermia over the left scapula.
Interpretation of the Thermal Images
The areas of hyperthermia indicate increase in circulation due to inflammation, infection, or malignancy. The areas of hypothermia indicate decrease in circulation due to neuropathy, atrophy, or vasoconstriction.
Additional Diagnostics
When the thermographic image was shown to the client she remarked: “You know, I touched that exact spot a few weeks ago and it seemed painful.”
A radiographic study was recommended and the client readily complied.
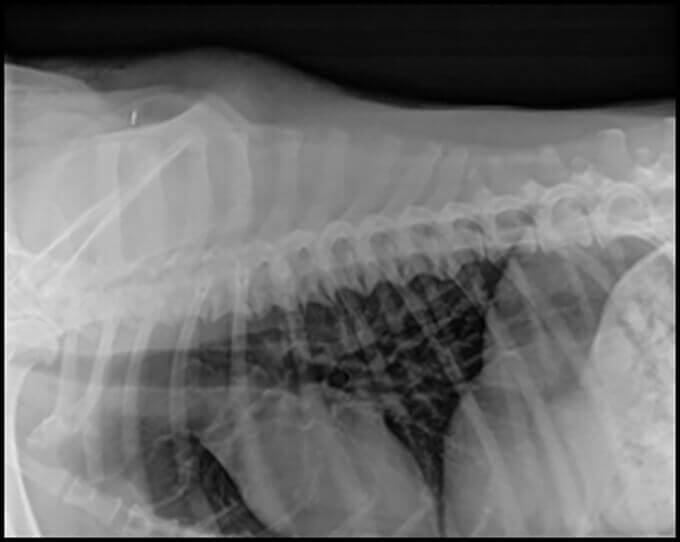
Radiographs indicated spondylosis deformans of the thoracic spine (Fig. 3).
Treatment Recommendation
Pharmaceutical pain management and nutraceuticals were prescribed.
Infrared Digital Thermal Imaging Provided:
- Early detection of a disorder that was not palpated during the physical exam or mentioned in the history.
- Client education and understanding allowing immediate compliance to further diagnostics.
- Baseline information for monitoring the patient’s response to the treatment plan.